Don't Get Caught Short: Medicare's Coverage for Incontinence Products Explained

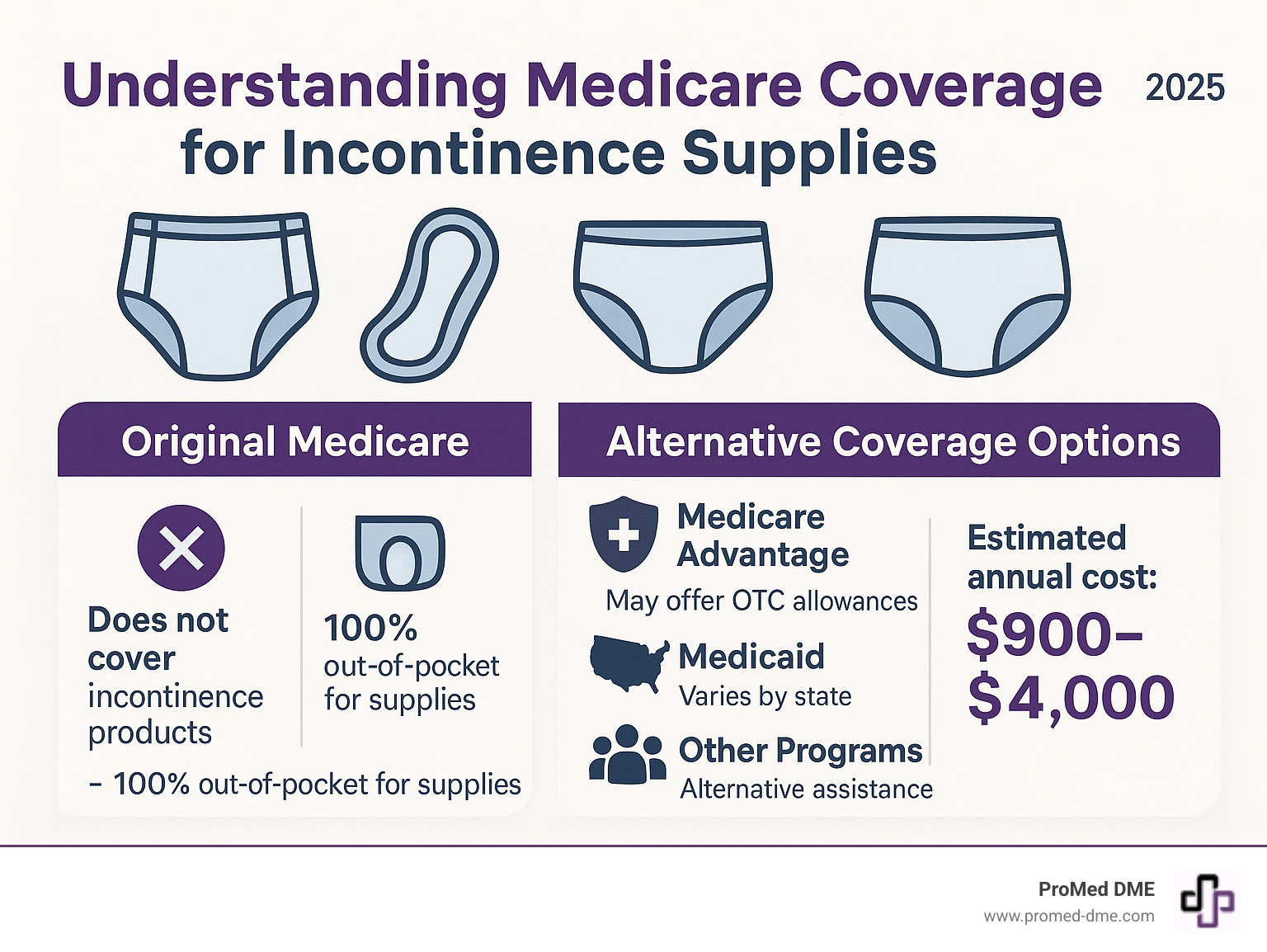
Understanding Medicare Coverage for Incontinence Supplies
Incontinence products medicare coverage can be confusing for the millions of Americans dealing with bladder control issues. The short answer? Original Medicare (Parts A and B) does not cover disposable incontinence supplies like adult diapers, pads, or protective underwear.
Here's what you need to know:
Original Medicare Coverage:
- Does NOT cover: Adult diapers, bladder control pads, protective underwear, or other absorbent products
- Does cover: Some durable medical equipment like catheters, bedside commodes, and grab bars (when medically necessary)
- Your cost: 100% out-of-pocket for disposable incontinence supplies
Alternative Coverage Options:
- Medicare Advantage (Part C): Some plans offer over-the-counter allowances for incontinence supplies
- Medicare Part D: Covers medications for conditions causing incontinence (not the supplies themselves)
- Medicaid: Often covers incontinence products when medically necessary (varies by state)
If you're one of the more than one-third of U.S. adults affected by urinary incontinence, these costs can add up quickly. Annual expenses for incontinence supplies range from $900 to $4,000, making coverage a significant concern for many seniors.
The key is understanding that Medicare treats these products as personal care items rather than medical necessities. This classification means you'll need to explore other options or pay out of pocket.
Incontinence products medicare terms explained:
- Does Medicare Cover Durable Medical Supplies
- Medical Supplies Medicare Covers
- Medicare Medical Supplies
The Bottom Line on Original Medicare (Part A & Part B)
Here's the reality about incontinence products medicare coverage that every senior needs to know: Original Medicare simply doesn't cover the supplies you probably need most.
Original Medicare has two main parts - Part A covers hospital care, and Part B handles medical insurance. While these programs are lifesavers for many medical expenses, they draw a hard line when it comes to absorbent incontinence products.
The reason? Medicare classifies adult diapers, bladder control pads, and protective underwear as personal care items rather than medical necessities. They're not considered Durable Medical Equipment (DME) either, which means you'll pay 100% of the costs out of your own pocket.
This can feel pretty unfair, especially when you're dealing with annual costs that can range from $900 to $4,000. Many people assume that since incontinence is a medical condition, the supplies would naturally be covered. Unfortunately, Medicare's classification system treats these items more like toiletries than medical devices.
The official Medicare website makes this crystal clear - incontinence supplies & adult diapers are not covered benefits. It's frustrating, but knowing this upfront can help you plan better.
What Incontinence-Related Items Does Part B Cover?
While disposable incontinence products medicare coverage is off the table, don't lose hope entirely. Medicare Part B does step up to cover certain durable medical equipment that can help manage bladder control issues - as long as they're medically necessary and prescribed by your doctor.

Catheter supplies are probably the most significant coverage area. If you need internal or external catheters due to urinary retention or permanent incontinence, Part B may cover these along with related supplies like leg bags and drainage bags. Medicare typically covers up to 35 male external catheters per month, and they even approved coverage for the PureWick urine collection system in 2024. After meeting your Part B deductible, Medicare usually covers 80% of the approved cost.
Pelvic floor stimulators can also qualify for coverage. These devices help strengthen the muscles that control bladder function, and if your doctor prescribes one as part of your treatment plan, Part B may pick up the tab.
Bedside commodes are another covered option for people who have difficulty getting to the bathroom due to medical conditions. While it's not exactly what you might think of as incontinence equipment, it serves an important function in managing bladder control issues.
Grab bars and raised toilet seats round out the coverage options. These safety items help people with mobility issues use the bathroom more safely, which can indirectly help with incontinence management.
The key to getting any of these items covered is working with your doctor to establish medical necessity and getting a proper prescription. You'll also want to use a Medicare-approved DME supplier to ensure smooth billing and coverage.
What About Treatments and Diagnosis?
Here's where Medicare really shines for incontinence issues - covering the medical side of things. While they won't pay for your pads, they will help with doctor visits, testing, and treatments.
Doctor visits for discussing bladder control problems are typically covered under Part B. Whether you're seeing your primary care physician, a urologist, or a gynecologist, these appointments fall under standard medical care.
Diagnostic testing is another area where Medicare steps in. Your doctor might order urinalysis to check for infections, urodynamic testing to measure bladder pressure and urine flow, or cystoscopy to examine your bladder and urethra. Pelvic exams and other lab work related to diagnosing your condition are also covered.
Treatment options covered by Medicare can include biofeedback therapy to help you learn better muscle control, and certain surgical procedures when medically necessary. If you need hospital admission for surgery to resolve severe urological problems, Part A hospital insurance may cover those costs too.
The bottom line? Don't let embarrassment keep you from talking to your doctor about bladder control issues. Getting a proper diagnosis is the first step toward finding treatments that Medicare will help pay for. Your physician can identify whether your incontinence stems from infections, medication side effects, weak bladder muscles, or other treatable causes.
For comprehensive information about diagnosis and treatment options, the National Institute on Aging offers excellent resources on urinary incontinence in older adults.
Understanding Your Options for Incontinence Products Medicare Coverage
If you're feeling frustrated by Original Medicare's limitations when it comes to incontinence products medicare coverage, you're not alone. The good news? You have other options worth exploring. While Original Medicare might leave you paying out of pocket for supplies, Medicare Advantage plans and prescription drug coverage can sometimes fill in those gaps.

Think of it like shopping for a car. Original Medicare is your basic model – it gets you where you need to go, but it doesn't have all the bells and whistles. Medicare Advantage and Part D plans? Those are your upgraded options with extra features that might just include what you're looking for.
Navigating Medicare Advantage (Part C) for Incontinence Products Medicare Coverage
Here's where things get interesting. Medicare Advantage plans are run by private insurance companies, and they're required to cover everything Original Medicare does. But here's the kicker – they often throw in extra benefits that can make a real difference in your daily life.
Many Medicare Advantage plans include what's called an over-the-counter allowance. This is essentially a monthly or quarterly allowance you can use to purchase health and wellness products. And yes, some plans specifically include incontinence products medicare supplies like adult diapers, pads, and protective underwear in their approved items list.
But – and this is important – not all Medicare Advantage plans are created equal. The benefits vary quite a bit from plan to plan, even in the same area. One plan might give you $100 per quarter for OTC items including incontinence supplies, while another might not offer this benefit at all.
Your best bet is to check your plan's Evidence of Coverage document. This detailed guide spells out exactly what your plan covers, including any OTC allowances. If you're shopping for a new plan, don't be shy about calling and asking direct questions about incontinence supply coverage.
When these allowances do exist, they typically work pretty simply. You get a set dollar amount to spend on approved items from a catalog or participating retailers. No prescription needed – just stick to the approved list and stay within your allowance.
How Medicare Part D Relates to Incontinence
Now, Medicare Part D won't help you buy adult diapers or pads – let's be clear about that upfront. But it plays a crucial role in managing the prescription medications that can help with the underlying causes of incontinence.
Think about it this way: if your doctor prescribes medication for an overactive bladder or antibiotics to treat a urinary tract infection that's causing temporary incontinence, Part D steps in to help cover those costs. These medications can sometimes reduce your symptoms significantly, potentially decreasing how many supplies you need.
The key is understanding your plan's formulary – that's the official list of covered drugs. Each Part D plan has its own formulary with different pricing tiers and copays. Before choosing a plan, make sure any incontinence-related medications you might need are covered and affordable under that plan's structure.
While Part D won't solve the supply cost issue directly, it can be invaluable for addressing the root causes of your incontinence. And sometimes, the right medication can make a bigger difference than you'd expect.
Alternative Paths to Coverage for Incontinence Supplies
When Original Medicare doesn't cover the incontinence products medicare supplies you need, it's natural to feel frustrated. The good news? There are other doors to explore that might help lighten the financial load of managing incontinence.

Medicaid and Dual-Eligible Coverage
Here's where things get more hopeful. Medicaid, the joint federal and state program for people with limited income and resources, often does cover incontinence supplies. Unlike Medicare's strict classification of these items as "personal care," Medicaid typically recognizes them as medical necessities when prescribed by a doctor.
The key thing to understand is that Medicaid programs vary quite a bit from state to state. While the federal government sets the basic framework, each state gets to decide its own eligibility rules and what supplies they'll cover. In most states, if your doctor documents your incontinence diagnosis and prescribes specific supplies, Medicaid will often cover adult diapers, protective underwear, bladder control pads, and underpads (chux).
Now, if you're lucky enough to qualify for both Medicare and Medicaid - what's called being "dually eligible" - you've hit the coverage jackpot for incontinence products medicare. Here's how it works: Medicare covers what it covers, and Medicaid steps in to fill the gaps. So while Original Medicare might cover 80% of that bedside commode after your deductible, Medicaid picks up your 20% share. More importantly for incontinence supplies, when Medicare says "no coverage," Medicaid often says "we've got you covered."
The best way to find out what's available in your area is to contact your state Medicaid office. They'll have the most current information about eligibility requirements and covered supplies in your specific state.
Other Financial Assistance Programs
Beyond Medicaid, there's a whole network of programs and organizations that understand the real financial burden of incontinence supplies. You just need to know where to look.
If you're a veteran, the Veterans Affairs (VA) system might be your answer. The VA often provides incontinence supplies as part of healthcare benefits, especially if your condition is service-connected or if you're enrolled in their healthcare system.
Here's something many people don't know: the National Diaper Bank Network isn't just for babies. Many local diaper banks that are part of this network also distribute adult incontinence products to families and individuals who need them. It's worth searching their website to see if there's a participating diaper bank near you.
Your local senior center can be a goldmine of information. These centers often know about community resources, local charities, and state programs that can help with medical supplies. The staff there deals with these questions regularly and can point you toward resources you might never have found on your own.
Some states run their own assistance programs specifically for medical supplies, separate from regular Medicaid benefits. These programs are designed to help low-income individuals or those with disabilities get the supplies they need.
If you're caring for someone with incontinence, the National Family Caregiver Support Program might offer grants or resources that can help offset costs. This program, run by the Administration for Community Living, is specifically designed to support family caregivers with various services and sometimes financial assistance.
Don't be embarrassed to ask for help. A simple online search for "incontinence supply assistance" plus your city or state name can uncover local resources you never knew existed. Many organizations are specifically there to help people steer exactly these kinds of challenges.
Frequently Asked Questions about Medicare and Incontinence Supplies
We understand that navigating incontinence products medicare coverage can feel overwhelming, especially when you're already dealing with a challenging health condition. You're not alone in having questions—we hear these same concerns from people every day. Let's tackle the most common questions with straightforward, honest answers.
Does Medicare pay for Depends or other adult diapers?
Here's the reality: Original Medicare (Parts A and B) does not cover disposable absorbent products like adult diapers, including popular brands like Depends. Medicare views these items as personal hygiene products rather than medical equipment, which means you'll pay 100% of the cost out of pocket.
We know this isn't the news you wanted to hear, especially when these supplies can cost thousands of dollars each year. However, there's a potential bright spot: some Medicare Advantage (Part C) plans offer over-the-counter allowances that can be used for incontinence supplies.
The key word here is "some"—not all Medicare Advantage plans include this benefit. If you're currently shopping for a plan or considering switching during the enrollment period, it's worth asking specifically about OTC allowances for incontinence products. Each plan has different benefits, so what one plan covers, another might not.
Are incontinence supplies a tax-deductible medical expense?
This is actually a smart financial question that many people don't think to ask. If your doctor prescribes incontinence supplies for a specific medical condition, the costs may qualify as tax-deductible medical expenses.
The IRS allows you to deduct medical expenses that exceed a certain percentage of your Adjusted Gross Income. For incontinence products medicare doesn't cover to be deductible, they need to be primarily for treating or preventing a medical condition. A prescription from your doctor or a letter of medical necessity stating that these supplies are essential for managing your condition would provide the documentation you'd need.
However, tax laws are complex and change regularly. We strongly recommend consulting with a tax professional who can look at your specific situation—your income, other medical expenses, and current tax regulations—to determine if you can benefit from this deduction.
What are the first steps if I'm experiencing incontinence?
The most important step is talking to your doctor. We understand this conversation might feel embarrassing, but here's something that might surprise you: incontinence affects more than one-quarter to one-third of U.S. adults, according to the American Urological Association. Your healthcare provider has helped many patients with this exact issue.
Your doctor plays a crucial role in several ways. First, they can diagnose the underlying cause of your incontinence through tests that Medicare Part B typically covers, such as urinalysis, urodynamic testing, or pelvic exams. Incontinence isn't just "getting older"—it can stem from treatable conditions like urinary tract infections, constipation, medication side effects, or weak pelvic floor muscles.
Once they identify the cause, your doctor can recommend treatments that Medicare may help cover. This might include bladder training techniques, pelvic floor exercises, medications for overactive bladder (covered by Medicare Part D), or medical devices like catheters or pelvic floor stimulators (potentially covered by Medicare Part B when medically necessary).
Perhaps most importantly for coverage purposes, your doctor can provide the medical necessity documentation that's required for potential insurance coverage through Medicaid, Medicare Advantage plans, or even tax deductions. Without this medical documentation, you'll have fewer options for financial assistance.
Don't let embarrassment keep you from getting help. Addressing incontinence early can improve your quality of life significantly and may prevent complications like skin irritation or infections. Plus, the sooner you have a proper diagnosis and treatment plan, the sooner you can explore all your coverage options for managing this condition effectively.
Conclusión
Finding your way through incontinence products medicare coverage can feel overwhelming, and honestly, we get it. The reality is that Original Medicare leaves you paying for absorbent supplies entirely out of your own pocket – something that can add up to thousands of dollars each year.
But here's what we want you to remember: you're not without options.
Yes, Original Medicare has its limitations when it comes to adult diapers and pads. The system treats these as personal care items rather than medical necessities, which means 100% out-of-pocket costs for disposable products. However, Medicare does step up when it comes to the medical side of things – covering your doctor visits, diagnostic tests, and essential durable medical equipment like catheters and bedside commodes.
The real game-changer often lies in Medicare Advantage plans. Many of these plans offer over-the-counter allowances that can help cover incontinence supplies. It's not a guarantee, but it's definitely worth investigating during your next enrollment period.
Medicaid emerges as perhaps the most valuable resource for many people dealing with incontinence. If you qualify – especially if you're eligible for both Medicare and Medicaid – you might find that Medicaid covers exactly what Medicare won't. State programs vary, but many do cover medically necessary incontinence products when prescribed by your doctor.
Don't overlook the smaller programs either. Local diaper banks, veteran benefits, and community assistance programs can provide real relief when you need it most.
The bottom line? Managing incontinence effectively requires both good medical care and smart navigation of the coverage landscape. Start with your doctor – they're your best ally in getting the medical documentation you need and exploring treatments that Medicare will cover.
At ProMed DME, we understand how frustrating these coverage gaps can be. While we can't change Medicare's policies on disposable products, we can help you get the durable medical equipment you're entitled to under Part B. Our team includes a dedicated nurse who can answer your questions and help you understand what's covered. We work with most insurance plans and offer free shipping nationwide, making it easier to get the medical supplies you need without the hassle.
Ready to explore what medical supplies Medicare might cover for your situation? Explore your medical supply options with ProMed DME today.
Recursos y artículos relacionados
Manténgase informado con las entradas de nuestro blog informativo.
Descubra las ventajas de ProMed
y pruebe nuestros productos
Ofrecemos envío gratuito y un legendario servicio de atención al cliente para garantizar que reciba los
mejores productos de DME para sus necesidades.